Portell Discusses the Treatment of Relapsed/Refractory CLL
During a virtual Case Based Peer Perspectives event, Craig A. Portell, MD, discussed how he would go about treating a patient case with chronic lymphocytic leukemia.
Craig A. Portell, MD

During a virtual Case Based Peer Perspectives event, Craig A. Portell, MD, associate professor, Division of Hematology/Oncology, University of Virginia Health, Charlottesville, Virgina, discussed how he would go about treating a patient case with chronic lymphocytic leukemia (CLL). He also highlighted the data supporting his treatment decisions and the role of minimal residual disease (MRD) testing in patients with CLL.
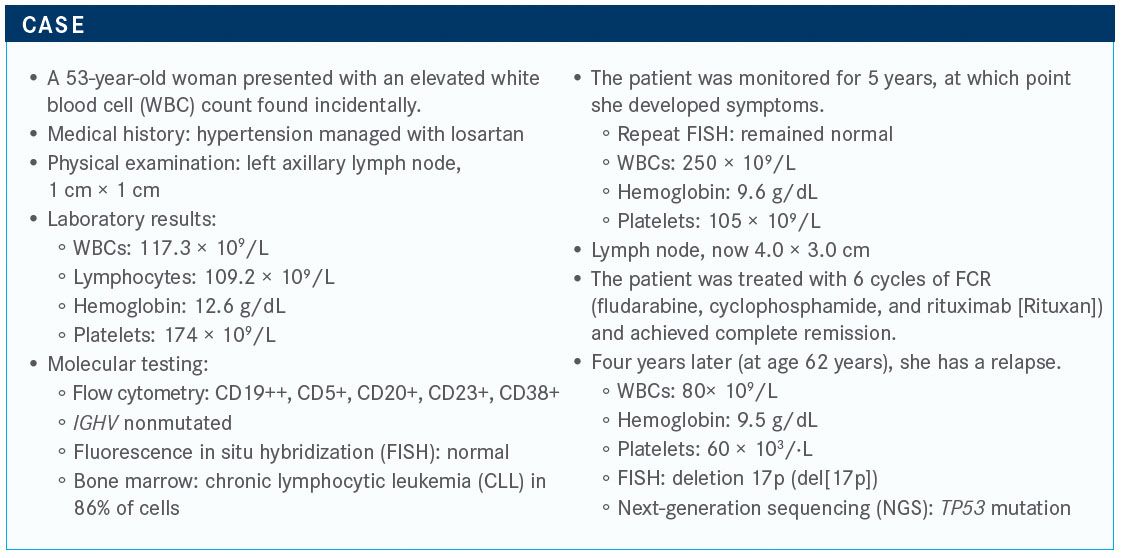

Targeted Oncology™: What are the data supporting this choice of therapy in patients with previously treated for CLL?
PORTELL: The RESONATE study [NCT01578707] randomized patients to ofatumumab [Arzerra] versus ibrutinib [Imbruvica], but the patients on ofatumumab were allowed to cross over.1 It was a 1:1 randomization of close to 400 patients, and those with del(17p) were allowed on this study.
The 6-year progression-free survival [PFS] rate…showed clear improvement [with ibrutinib] over ofatumumab [HR, 0.133; 95% CI, 0.099-0.178].
When looking at the genomic makeup, patients treated with ibrutinib showed no difference between IGHV mutated or unmutated for PFS. Del(17p) versus del(11q) versus neither showed [that patients with] del(11q) tend to do better with these novel agents than patients with del(17p). The median PFS hadn’t been reached in that cohort.
There was no difference in overall survival [OS] [between the 2 agents], although remember, crossover was allowed here, and a lot of censoring happened early on with the ofatumumab arm, probably related to the crossover.
The adverse events [AEs] were listed over time, which is an important point. Neutropenia tended to peak early with ibrutinib, as do infections, although there is a still a reasonable minority of patients who develop infections while they continue on ibrutinib.
One interesting finding is that hypertension tended to happen as a later event with these BTK [Bruton tyrosine kinase] inhibitors, which is something that’s been played out before. There was slightly more hemorrhage seen later with the BTK inhibitors too.
How have other trials investigated therapies for this patient population?
The ASCEND study [NCT02970318] compared acalabrutinib [Calquence] monotherapy with idelalisib [Zydelig] or bendamustine [Treanda] and rituximab and did allow crossover to acalabrutinib if there was confi rmed progression, which was considered the standard-of-care arm at the time.2 They allowed patients with del(17p), and they were stratifi ed appropriately, as was the number of prior therapies.
The median PFS for the acalabrutinib arm was not reached, but for the idelalisib and rituximab [arm] or the bendamustine and rituximab [arm], it was about 16.5 months, with a median follow-up of 16.1 months [HR, 0.31; 95% CI, 0.20-0.49; P < .0001]. OS was not recorded because it was not yet mature. The PFS by subgroup showed that most patients were favoring the acalabrutinib.
Looking at safety, serious AEs were seen with the acalabrutinib arm, including some grade 5 AEs. Headaches were also more common with acalabrutinib than any of the other agents.
Which studies have looked at combination therapy for these patients?
The MURANO data [NCT02005471] evaluated bendamustine and rituximab versus venetoclax [Venclexta] and rituximab in a 1:1 randomization; patients with del(17p) were allowed [to enroll].3 It showed an improvement in 4-year PFS with venetoclax against bendamustine [HR, 0.19; P < .0001]. There was a trend toward a sustained OS advantage, with an 85.3% 4-year OS rate with venetoclax and 66.8% with bendamustine [HR, 0.41; P <.0001].
The interim analyses showed improvement with venetoclax in all the subgroups. Secondary end points pointed to improved overall response, as well as a deeper remission rate and undetectable minimal residual disease [MRD] rate compared with bendamustine.
There was slightly more neutropenia in the venetoclax group. About 58.8% had some degree of grade 3/4 neutropenia with venetoclax, but there was more febrile neutropenia with the bendamustine and rituximab.
Do you routinely use MRD testing in your practice? How would it affect your treatment of this patient?
I’ve done it in a few situations, and it’s mostly when I’m considering a patient for transplant [and I’m worried about it]. We know that if a patient is in the deepest remission possible prior to going to transplant, their transplant outcomes are better. I have used MRD to guide when it’s time to go forward with transplant, and that’s pretty much the only place I’ve used it.
If I was considering transplant for a patient like this, I may consider venetoclax because I would get a deeper MRD-negative remission over ibrutinib.…If transplant is off the table, then I think ibrutinib and venetoclax are both reasonable. That would be my approach.
When you get MRD testing, what is your preferred method?
In my thoughts, if I’m taking someone to transplant and using MRD as that measure, I would get fl ow cytometry [over] the bone marrow [biopsy], because they’re getting bone marrow for the transplant [anyway].
Refereneces
1. Byrd JC, Hillmen P, O’Brien S, et al. Long-term follow-up of the RESONATE phase 3 trial of ibrutinib vs ofatumumab. Blood. 2019;133(19):2031 2042. doi:10.1182/ blood-2018-08-870238
2. Ghia P, Pluta A, Wach M, et al. Acalabrutinib vs rituximab plus idelalisib (idR) or bendamustine (BR) by investigator choice in relapsed/refractory (RR) chronic lymphocytic leukemia: phase 3 ASCEND study. Hematol Oncol. 2019;37(52):86-87. doi:10.1002/hon.54_2629
3. Seymour JF, Kipps TJ, Eichorst BF, et al. Venetoclax plus rituximab is superior to bendamustine plus rituximab in patients with relapsed/ refractory chronic lymphocytic leukemia - results from pre-planned interim analysis of the randomized phase 3 MURANO study. Blood. 2017;130 (suppl 1):LBA-2. doi: 10.1182/blood.V130. Suppl_1.LBA-2.LBA-2